General Eye Care
Your eye exam will evaluate both your vision and the health of your eyes. Before the actual eye exam, you will meet with an ophthalmic technician who will take your medical and eye history and perform visual screening tests and administer drops to dilate your pupils before meeting with the physician. During your exam, you will likely have all or most of the following eye tests:
- Eye muscle movement to test muscle strength and control
- Cover test to examine how well your eyes work together
- External exam and pupillary reactions to test your pupil's reaction to light, and the whites of the eyes and eyelid position
- Visual acuity to test your ability to read eye charts in the distance and up-close
- OPD/Auto-Refraction to determine the approximate lens required for your to achieve the best vision
- Subjective refraction testing to determine your exact lens prescription
- Slit lamp to detect eye diseases and disorders by examining the cornea, iris, lens and anterior chamber
- Retinal examination to examine the retina, retinal blood vessels, optic nerve head and mac ula
- Pupil dilation* to examine the complete inside of your eyes with specialized 3D view instruments
*Please Note: The pupil-enlarging drops for this part of your eye exam start to work after about 20 minutes, making your eyes more sensitive to light and blurring your vision somewhat. These effects may last for several hours, so it’s important to bring a pair of sunglasses to your exam if you are planning to drive yourself home. Some of our patients feel safer bringing a driver so they do not need to drive home afterward with their eyes dilated.
Having your child's eyes and vision examined by an optometrist or ophthalmologist early in their visual development is best. Parents should not wait until their children report visual problems. With some visual skills reaching full development at about 5 years of age, correction after this point becomes more difficult. Visual defects discovered before this age can be treated; therefore it is vital for parents to schedule regular eye examinations as recommended by their Pediatrician, their Eye care Professional and the American Optometric Association.
Parents should pay attention to these indications that a child might be experiencing visual problems:
- Squinting
- Reading from books held unusually close to the face
- Eyes pointing in different directions
- Twisting or tilting of the head to favor one eye
- Complaints of headaches and dizziness
- Blurred or double vision
- Frequent blinking or rubbing of eyes
- Inability to judge distance properly (bumping into things)
- Poor school and athletic performance
With that in mind, here are a few important points to keep in mind before you send your child out to play:
- UV rays are greatest when the sun is at its highest in the sky between 10 am and 4pm.
- Exposure is greatest from May through August in the United States
- UV levels are greater in wide open spaces, especially when highly reflective surfaces are present, like snow and sand.
The polarization of light occurs when light is reflected off of certain surfaces such as snow, cement and water. This means that vertical light waves are absorbed while horizontal light waves bounce off the surface, creating glare. Polarized lenses reduce glare, provide 100% protection from harmful UV rays, increase visual acuity and decrease eye strain.
Children can benefit greatly from polarized lenses because they are frequently exposed to considerable sources of reflected glare and harmful UV rays during outdoor activities. Getting into the routine of wearing protective sunglasses should begin at a young age and is encouraged as a life-long habit. Prescription sunglasses are available for Children with corrective lenses to help protect their eyes.
Eye Health for Adults:
An annual eye exam is one of the most important diagnostic and preventative measures you can take to protect your vision and health.
If you are in a higher-risk category for eye disease or complications, such as diabetes your eye doctor will recommend more frequent exams. If you notice a change in your vision or receive an injury to your eye, you should contact your eye care professional immediately.
The most common vision problems are refractive errors, more commonly known as nearsightedness, farsightedness, astigmatism and presbyopia. Refractive errors occur when the shape of the eye prevents light from focusing directly on the retina. The length of the eyeball (either longer or shorter), changes in the shape of the cornea, or aging of the lens can cause refractive errors. Most people have one or more of these conditions.
- Amblyopia (lazy eye)
- Astigmatism (irregular curvature of the front of the eye)
- Myopia (nearsighted)
- Hyperopia (farsighted)
- Myopia
- Presbyopia (also known as Aging eyes)
- Strabismus (crossed eyes)
What is a refraction?
Refraction is the bending of light as it passes through one object to another. Vision occurs when light rays are bent (refracted) as they pass through the cornea and the lens. The light is then focused on the retina. The retina converts the light-rays into messages that are sent through the optic nerve to the brain. The brain interprets these messages into the images we see.
What are the different types of refractive errors?
The most common types of refractive errors are nearsightedness, farsightedness, astigmatism and presbyopia. Nearsightedness (also called myopia) is a condition where objects up close appear clearly, while objects far away appear blurry. With nearsightedness, light comes to focus in front of the retina instead of on the retina.
Farsightedness (also called hyperopia) is a common type of refractive error where distant objects may be seen more clearly than objects that are near. However, people experience farsightedness differently. Some people may not notice any problems with their vision, especially when they are young. For people with significant farsightedness, vision can be blurry for objects at any distance, near or far.
Astigmatism is a condition in which the eye does not focus light evenly onto the retina, the light-sensitive tissue at the back of the eye. This can cause images to appear blurry and stretched out.
Presbyopia is an age-related condition in which the ability to focus up close becomes more difficult. As the eye ages, the lens can no longer change shape enough to allow the eye to focus close objects clearly.
Who is at risk for refractive errors?
Presbyopia affects most adults over age 35. Other refractive errors can affect both children and adults. Individuals that have parents with certain refractive errors may be more likely to get one or more refractive errors. What are the signs and symptoms of refractive errors?
Blurred Vision is the most common symptom of refractive errors. Other symptoms may include:
- Double vision
- Haziness Glare or halos around bright lights
- Squinting
- Headaches
- Eye strain
Diabetes & Vision:
Diabetes is a disease that causes your body to not use or store sugar properly. When your blood sugar gets too high, it can damage your eye by weakening or swelling the tiny blood vessels in the retina. This damage may lead to diabetic retinopathy. This disorder usually occurs in both eyes and dims or obliterates vision temporarily.
Diabetes may lead to new blood vessel growth on top of the retina. These blood vessels can develop into scar tissue, pulling the retina away from the back of the eye. This is called retinal detachment, and can lead to blindness if untreated. Additionally, irregular blood vessels can grow on the iris, leading to glaucoma.
Everyone who has diabetes is at risk for developing diabetic retinopathy. You may not notice any change in your vision in its early stages, which is why regular eye examinations are extremely important. What is diabetic eye disease?
What is Diabetic Eye Disease?
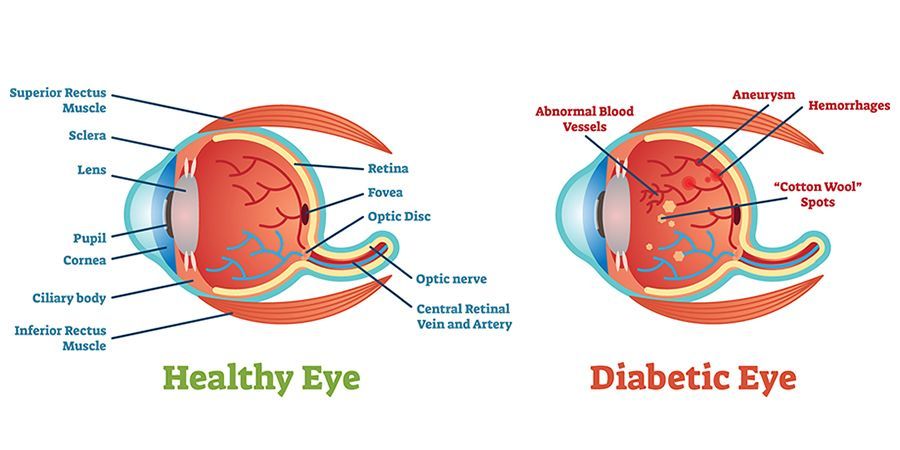
Diabetic eye disease is a group of eye conditions that can affect people with diabetes.
- Diabetic retinopathy affects blood vessels in the light-sensitive tissue called the retina that lines the back of the eye. It is the most common cause of vision loss among people with diabetes and the leading cause of vision impairment and blindness among working-age adults.
- Diabetic macular edema (DME). A consequence of diabetic retinopathy, DME is swelling in an area of the retina called the macula.
Diabetic Eye Disease also includes Cataract and Glaucoma:
- Cataract is a clouding of the eye’s lens. Adults with diabetes are 2-5 times more likely than those without diabetes to develop cataract. Cataract also tends to develop at an earlier age in people with diabetes.
- Glaucoma is a group of diseases that damage the eye’s optic nerve—the bundle of nerve fibers that connects the eye to the brain. Some types of glaucoma are associated with elevated pressure inside the eye. In adults, diabetes nearly doubles the risk of glaucoma.
- Visual acuity testing. This eye chart test measures a person’s ability to see at various distances.
- Tonometry. This test measures pressure inside the eye.
- Optical coherence tomography (OCT). This technique is similar to ultrasound but uses light waves instead of sound waves to capture images of tissues inside the body. OCT provides detailed images of tissues that can be penetrated by light, such as the eye.
A comprehensive dilated eye exam allows the doctor to check the retina for:
- Changes to blood vessels
- Leaking blood vessels or warning signs of leaky blood vessels, such as fatty deposits
- Swelling of the macula (DME)
- Changes in the lens 5. Damage to nerve tissue









